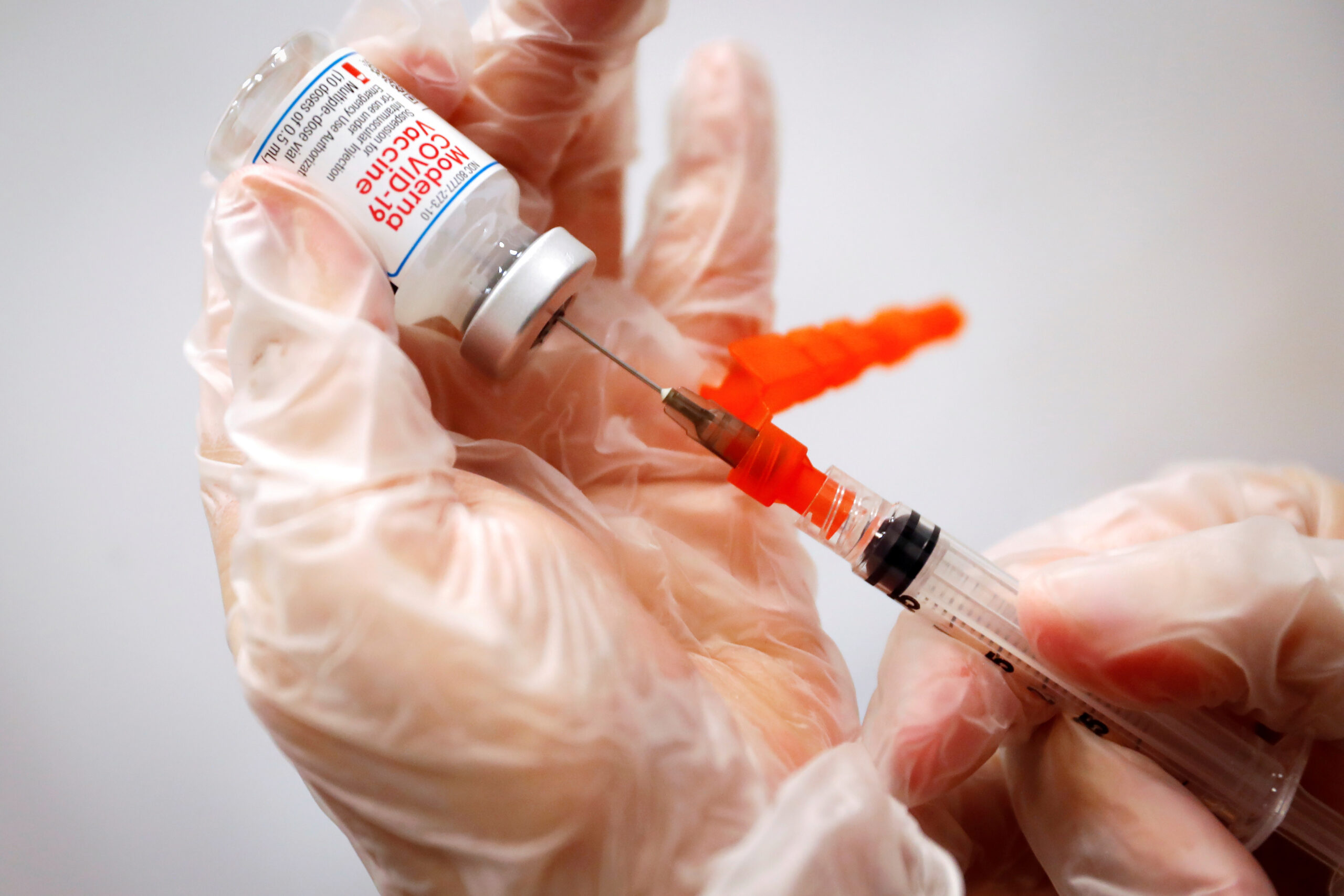
An infectious disease expert answers questions on COVID-19 breakthrough cases, vaccines during pregnancy and booster shots
September 8, 2021With coronavirus hospitalizations in Texas hovering just below the pandemic’s winter peak, Texans are again grappling with how to deal with the virus in their day-to-day lives.
Last week, the Texas Education Agency announced that at least 45 small school districts shut down in-person classes due to high COVID-19 numbers. On top of that, major metropolitan hospitals are halting elective surgeries — as they did during prior surges when hospitals filled up with COVID patients.
Although vaccines have slightly changed the calculus on safety protocols, many of the same factors that drove the winter surge are also driving the current wave of cases.
The Texas Tribune spoke with Dr. James Cutrell, an associate professor at the University of Texas Southwestern Medical Center who specializes in COVID-19 treatment, to answer questions about masks, vaccinations and breakthrough cases. Cutrell completed a fellowship in infectious diseases in 2013 at UT Southwestern and now is the director of the adult fellowship program in infectious diseases.
If you get vaccinated, do you still have to wear a mask?
Although the COVID-19 vaccines continue to provide very good protection, particularly against severe disease, hospitalization or death, there remains a risk of milder infection in those who are fully vaccinated.
Moreover, if infected, those who are fully vaccinated are able to transmit that infection to others, although their overall risk of transmission is lower than those who are unvaccinated. In order to reduce both the personal risk of infection and risk of spreading it to others, masking can be one effective strategy to protect yourself and others.
Therefore, the current CDC recommendations are that fully vaccinated individuals should continue to wear a mask when in public indoor spaces if they live in an area of substantial or high COVID-19 transmission. The definition of an area of substantial or high COVID-19 transmission is more than 50 cases per 100,000 people or a test positivity rate greater than 8%. This would currently include many areas of the country, including Texas.
How common are breakthrough cases for vaccinated people? Is the state tracking that?
Although early data from the end of April 2021 reported that breakthrough cases were very uncommon (about 0.01% among the first 100 million Americans vaccinated), breakthrough cases have become more common as community cases and transmission with the delta variant have risen across the country.
Precise estimates of the frequency of breakthrough cases are not known because since May 2021 the CDC has primarily been tracking breakthrough cases only in those who are hospitalized or die. There are some states that have continued to track the rates of breakthrough cases, but Texas is only tracking hospitalized or fatal cases due to COVID-19 breakthrough infections.
The CDC is conducting focused studies in 10 states through the Emerging Infections Program to determine better estimates of the overall rate of breakthrough cases during the current delta variant surge, including milder disease and infection.
What are the timelines around expanding eligibility for the vaccine? When can children under 12 get it?
Current clinical trials are ongoing, evaluating the safety and efficacy of the mRNA vaccines (Pfizer and Moderna) for children under 12.
We expect that the data in the group of children ages 5-11 will be submitted to the FDA at some point in the early to mid-fall for review. There is less certainty around how long the FDA review process will take.
The CDC is recommending that pregnant women get vaccinated. Is there any research on how the vaccine affects pregnancy?
The CDC recently strengthened their recommendation of the COVID-19 vaccines for those who are pregnant, breastfeeding or considering pregnancy. This is based on increasing data showing that the vaccines are safe in pregnancy, with no signals of increased risk of miscarriage, preterm birth or other adverse pregnancy outcomes.
Additionally, the vaccine has proven effective at reducing the risk of COVID-19 infection in pregnancy.
Finally, there is a growing body of evidence showing that pregnant women who develop COVID-19 have a higher risk of severe disease leading to hospitalization or death and also a higher risk of pregnancy complications due to the infection. For all of these reasons, the benefits of COVID-19 vaccination in pregnancy strongly outweighs potential risks or side effects.
I live with someone who is immunocompromised. They already got their Pfizer booster. Should I get the booster early, too?
Currently the additional third doses (boosters) are only being administered to those who are moderately to severely immunocompromised. Those who are close or household contacts of an immunocompromised individual are not yet recommended to receive a booster.
At this point, the most important things for those who are close contacts to an immunocompromised patient are to be sure they are fully vaccinated (with their first two vaccine doses) and to be sure that they are wearing masks and taking other precautions when in public settings to minimize their risk of developing COVID-19 and spreading it to their loved one.
Are the mRNA boosters developed specifically for the delta variant? I’ve seen reports that Moderna and Pfizer are working on vaccines that target the delta variant.
The current boosters being administered and considered are the original mRNA vaccine, which was targeted for the original SARS-CoV-2 virus. These vaccines still show good efficacy against the delta variant, particularly in preventing more severe disease.
Clinical trials of updated mRNA vaccines, which are designed specifically to target the delta variant, began in August 2021, so in the future there will likely be boosters approved specifically for that variant.
When will the Moderna and Johnson & Johnson vaccines get FDA approval?
Moderna completed its submission of data for full FDA approval in late August 2021. The FDA is reviewing under priority review so we expect that this fall it will be approved (for reference, it took 97 days from full submission of the Pfizer vaccine data to full approval). The Johnson & Johnson vaccine is expected to have its data submitted for full approval by the end of 2021.
This article was originally posted on An infectious disease expert answers questions on COVID-19 breakthrough cases, vaccines during pregnancy and booster shots


